 
Yearly mammograms are needed for the treated breast and the unaffected breast.There is a small risk of DCIS coming back or of invasive cancer developing in the future.(For more information see the brochure Radiotherapy.) Radiotherapy can cause side effects to the skin, breast tissue and other nearby tissues.Radiotherapy is typically given daily over a period of four to six weeks, requiring regular trips to the hospital for treatment.There is a 10–20% chance of needing a second operation to get clear margins (this will not be known until a week after surgery when the pathology results are available).Some DCIS may be left behind at surgery because it cannot always be seen on mammograms or felt by the surgeon.The radiotherapy significantly reduces the risk of DCIS or invasive cancer in the future.The surgery usually results in a good cosmetic result.The surgery is less extensive than mastectomy and the recovery is quicker.This is X-ray treatment that kills cancer cells and significantly reduces the risk of DCIS or invasive breast cancer developing in the remaining breast tissue in the future. Under general anaesthetic, the surgeon removes the area of DCIS and a small area of healthy tissue around it (the ‘surgical margin’).Īfter surgery, radiotherapy (radiation therapy) is given to the breast. Wide local excision (breast conservation surgery) and radiotherapy (radiation therapy) Each treatment has advantages and disadvantages. The surgeon can discuss the likelihood of invasive breast cancer with you before the operation. This is more likely if the area of DCIS is large or if it can be felt as a lump. 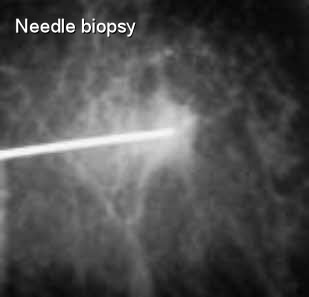
In around a quarter of cases, early invasive breast cancer (rather than only DCIS) is found in the final pathology. Sometimes, even when the core biopsy shows DCIS, areas of invasive breast cancer are seen when the whole area is removed by a surgeon and examined in detail by a pathologist. If this happens, DCIS has become invasive (or infiltrating) cancer, which in turn can spread to lymph nodes or to other parts of the body.ĭCIS is usually diagnosed on a core needle biopsy before surgery. If left untreated, they may spread out of the milk duct into the breast tissue. Occasionally women with DCIS may have a breast lump or nipple discharge. DCIS is usually diagnosed on a mammogram where it may be seen as specks of calcium (microcalcification). Invasive breast cancer can spread to other parts of your body. If left untreated, DCIS may develop into invasive breast cancer (cancer that moves beyond the milk ducts). It is sometimes also referred to as ‘pre-cancer’. This can be considered a very early form of breast cancer. As these cells are contained within the ducts and have not spread into the surrounding breast tissue (in situ), there is very little chance that the cells can spread into the lymph nodes or anywhere else in the body. Published by Oxford University Press on behalf of BJS Society Ltd.Ductal carcinoma in situ (DCIS) occurs when some of the cells that line a group of milk ducts within your breast have started to become cancer cells. Well-designed randomized controlled trials are required to establish fully the necessity of SLNB for patients diagnosed with DCIS. While aggressive clinicopathological parameters may guide SLNB for patients with DCIS, the absolute and relative risk of SLNB+ for DCIS is less than 5 per cent and 1 per cent, respectively. 0.80 to 2.23 P = 0.270, I2 = 0 per cent) all trended towards significance in predicting SLNB+. The likelihood of having SLNB+ for DCIS was less than 1 per cent (o.r. Of these, 72.5 per cent of patients underwent SLNB (3156 of 4356 patients) and 4.9 per cent had SLNB+ (153 of 3153 patients). Overall, 16 studies including 4388 patients were included (mean patient age 54.8 (range 24 to 92) years). Characteristics predictive of SLNB+ were expressed as dichotomous variables and pooled as odds ratios (o.r.) and associated 95 per cent confidence intervals (c.i.) using the Mantel-Haenszel method. The aim was to establish the likelihood of having a positive SLNB (SLNB+) for DCIS and to establish parameters predictive of SLNB+.Ī systematic review was performed as per the PRISMA guidelines. Quantification of the necessity of upfront SLNB for DCIS requires investigation. The presence of an invasive component to DCIS mandates nodal evaluation through sentinel lymph node biopsy (SLNB). 
Ductal carcinoma in situ (DCIS) is a non-invasive disease and does not spread to axillary lymph nodes. Axillary lymph node status remains the most powerful prognostic indicator in invasive breast cancer. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
